
How to Have Fun in the Sun According to RCCA’s Dermatologic Oncologists
East Coast residents are no strangers to winter weather, and those long, chilly months tend to make time under the summer sun that much more appealing.
HIPAA Alert: Potential Data Breach Learn More
Questions on Oncology, Hematology and/or Infusion Clinical Services due to COVID-19 Crisis – CALL 833-698-1623
Important Information for Our Patients Regarding the Coronavirus.
RCCA Providing Area Cancer Patients with Access to Care During Coronavirus Outbreak
RCCA Offering Patients Virtual Visits During Coronavirus Pandemic
The New Jersey average of 22.2 new cases of melanoma per 100,000 people per year disguises a discrepancy in county rates, which show higher rates in the southern portion of the state — 8.2 cases per 100,000 in Hudson County ranging to 51.3/100,000 in Cape May County.
Additionally, Cape May, Atlantic, Monmouth and Sussex counties are experiencing an increase in cases, while the rate of new melanoma cases is stable in three-quarters of the state’s counties.
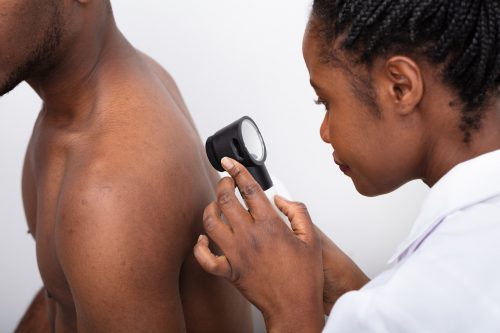
Melanoma: New Case Numbers and Trends in South Jersey
| County | Age-adjusted incidence rate per 100,000 people | Recent 5-year trend in incidence rate (average annual percent change) | Recent trend | Average annual case count |
| Atlantic | 27.1 | +1.6 | Rising | 92 |
| Burlington | 26.4 | +0.5 | Stable | 146 |
| Camden | 21.7 | +0.3 | Stable | 128 |
| Cape May | 51.3 | +3.3 | Rising | 77 |
| Cumberland | 16.4 | +1.3 | Stable | 28 |
| Gloucester | 27.2 | +0.7 | Stable | 91 |
| Ocean | 34.0 | +0.2 | Stable | 283 |
| Salem | 32.4 | -16.8 | Stable | 26 |
Source: National Cancer institute. State Cancer Profiles. Available at https://statecancerprofiles.cancer.gov/quick-profiles/index.php?statename=newjersey. Accessed May 7, 2021.
It would be easy to say the higher numbers in southern New Jersey are higher because of the amount of time spent on beaches or farms, but the answer is not that simple. In fact, it could come down to individuals in certain areas of the state being more diligent about having regular examinations, which in turn leads to an increase in diagnoses, said Stephen G. Wallace, a board-certified medical oncologist and hematologist who practices with Regional Cancer Care Associates LLC, or RCCA, in Moorestown.
That diligence also is key to successfully treating melanoma. “As with any cancer, the earlier you detect and treat melanoma, the lower the chance of it spreading to other parts of the body, and the greater the chance that it can be treated effectively with less-aggressive measures,” Dr. Wallace said.
Recognizing Melanoma
Whether you live in Mahwah or Margate, and whether your phone number begins with 609 or 201, having a skin examination on a regular basis is important, the cancer specialist notes.
Dr. Wallace said that regardless of area code or residence, it’s smart to conduct a self-examination once a month or so and to see a dermatologist if an unusual mole is found.
While conducting a self-examination, follow the ABCDE method, said Julianne W. Childs, DO, a board-certified medical oncologist and hematologist who practices with RCCA in Cape May Court House and Marmora.
She said to keep an eye out for one or more of the following characteristics, and if found, see a dermatologist:
Dr. Childs said that any mole that changes shape, color, size and/or elevation is especially concerning, even if the mole has been there for years.
“Having one or more of these features does not necessarily mean that a mole is a melanoma, but it absolutely means that it should be evaluated by a dermatologist,” Dr. Childs said. “One or more of these findings is not cause to panic, but it is reason to act.”
Dr. Childs said that melanoma may be deceiving in appearance. For instance, an individual may have something that looks like a scab, but once the scab falls off, another one returns, and it keeps growing. That is a sign a sign to see a dermatologist right away.
Dr. Childs discussed two other facts about melanoma:
Regular skin examinations with a dermatologist are a benefit to everyone, but they are especially important for individuals with the following risk factors, said Drs. Childs and Wallace:
Reducing Your Risk
These simple steps can go far toward keeping you — and your family — relatively safe from melanoma:
Limit sun exposure. Stay indoors between 10 a.m. and 2 p.m., when the sun is strongest.
Don’t let your children get sunburned. “The earlier in life sunburn happens, the greater the risk for melanoma later on,” Dr. Childs said.
Wear sunscreen with a sun protection factor (SPF) of 30 or higher when in the sun. Apply it thoroughly across exposed areas and keep reapplying sunscreen at no more than two-hour intervals during sustained exposure to the sun (for example, while on the beach, on the farm or at a job site). “You can’t apply sunscreen just once and then stay out in the sun for 10 hours and not expect to have a sunburn,” Dr. Childs said.
Wear protective clothing. Stylish summer clothes that block UV rays are widely available online and in chain sporting goods stores. Also, wear light colors, which reflect sunlight away from your body.
Avoid tanning salons. Just one indoor tanning session can increase your risk of melanoma by 20%, according to the American Academy of Dermatology (AAD). A single “tan in a can” also can raise your risk of two other skin cancers: squamous cell carcinoma and basal cell carcinoma, the AAD reports.
Advances in Treating Melanoma
Immunotherapies that enable the immune system to find and eliminate cancer cells, and targeted therapies that act on specific genetic proteins that cause abnormal cell growth, have drastically changed the prognosis for melanoma. Additionally, the continued development of experimental medications that lead to even more hope.
“Just 10 to 15 years ago, if we had a new patient with stage 4 melanoma, you couldn’t be very hopeful, nor could you offer many treatment options. The situation is far different today,” Dr. Wallace said.
“The immunotherapies we are able to employ now often drive the immune system to take over and counteract the disease, even after it’s become metastatic,” Dr. Childs said.
RCCA network medical oncologists are experts at evaluating and treating later-stage melanomas. The physicians regularly participate in clinical trials of treatments that target melanoma and other solid tumors and blood-based cancers. Patients typically are referred to an RCCA cancer specialist after their melanoma has been diagnosed, initially treated and staged by a dermatologist and dermatologic surgeon.
“We treat patients according to the best current evidence using the latest treatments,” Dr. Wallace said. “It’s a matter of knowing what treatment strategy is right for each patient and making sure they can take advantage of the best existing therapies.”
Dr. Childs and Dr. Wallace are among more than 80 oncology physicians and nurse clinicians practicing at 20-plus RCCA care centers throughout New Jersey, Connecticut, Massachusetts and the Washington, D.C., area. RCCA provides care to roughly 22,000 new cancer patients and 225,000 established patients each year, offering those patients immunotherapy, targeted treatment, cell-based therapy and other cutting-edge treatments and diagnostic modalities, as well as access to clinical trials. RCCA care centers also provide infusion services for patients with non-oncology conditions — such as multiple sclerosis, rheumatoid arthritis, Crohn’s disease and others — who are being treated with intravenously-administered medications.
For more information or to schedule an appointment,
call 844-346-7222. You can also schedule an appointment by calling the RCCA location nearest you.

East Coast residents are no strangers to winter weather, and those long, chilly months tend to make time under the summer sun that much more appealing.

One of the most effective ways to treat cancer is to harness the power of the body’s own immune system. This method is called immunotherapy.
If you or a loved one has been diagnosed with cancer, doctors can choose from many treatments to provide the best care possible for each

Regional Cancer Care Associates is one of fewer than 200 medical practices in the country selected to participate in the Oncology Care Model (OCM); a recent Medicare initiative aimed at improving care coordination and access to and quality of care for Medicare beneficiaries undergoing chemotherapy treatment.