
Deciding Where to Receive Cancer Care: RCCA Oncologists Outline Key 5 Considerations
“My uncle’s neighbor was diagnosed with the exact same cancer, I think, last year and his specialist has been wonderful. I’m going to get you
HIPAA Alert: Potential Data Breach Learn More
Questions on Oncology, Hematology and/or Infusion Clinical Services due to COVID-19 Crisis – CALL 833-698-1623
Important Information for Our Patients Regarding the Coronavirus.
RCCA Providing Area Cancer Patients with Access to Care During Coronavirus Outbreak
RCCA Offering Patients Virtual Visits During Coronavirus Pandemic
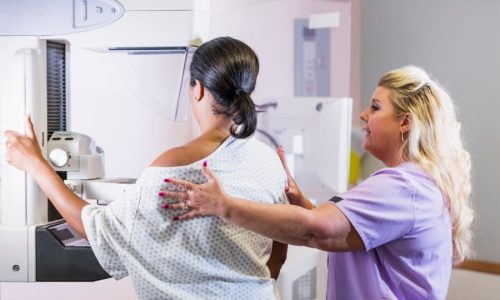
A screening mammogram is the type of breast imaging that most female patients are used to having. These are routine X-ray imaging tests used to detect possible signs of breast cancer. Screening mammograms are used for patients who do not have any signs or symptoms of breast cancer.
Typically, a screening mammogram doesn’t take more than 15 minutes. This type of imaging test is considered a form of preventive care per Affordable Care Act guidelines, so most insurance providers will cover screening mammograms at no cost to the patient. Most women should have an annual mammogram beginning at the age of 45. However, women may need to start regular screenings earlier if they have certain risk factors, such as a family history of breast cancer.
In contrast, diagnostic mammograms are performed when abnormalities are detected on a screening mammogram or when a patient has symptoms that might indicate cancer. These symptoms include:
A diagnostic mammogram usually takes longer than a screening mammogram, because the technologist will visualize the breast tissue from different angles and take more images. This can help determine if a patient’s symptoms are indicative of breast cancer. A diagnostic mammogram may be followed by other imaging tests, like a breast ultrasound.
Mammograms can be performed at a doctor’s office, hospital, or imaging center. Whether women require a screening or diagnostic mammogram, they will receive instructions from their provider on how to prepare for the test. For example, patients should not apply any lotions or creams around their chest or use deodorant under their arms prior to their appointment. Some of these products can show up as white spots on X-ray images, making the results more difficult to interpret.
During a screening mammogram, a breast imaging technologist will place the patient in the correct position in front of the mammography machine. Because they will be in a standing position throughout the exam, patients should notify their technologist if they have difficulty standing unassisted.
Before the exam, a patient will have to undress above the waist and put on a medical gown. An imaging technologist will position the patient’s breasts, one at a time, between two imaging plates. The patient will feel pressure as the plates are compressed while the machine takes images. This can be uncomfortable, but it only takes a few minutes.
The process for a diagnostic mammogram is similar. However, the technologist will take more pictures and may capture magnified images of any areas of concern. Some diagnostic mammograms use a technology called tomosynthesis, or 3D mammography. This is a type of digital X-ray that can be used to provide more detailed information about the breast tissue. If a woman has a 3D mammogram, she may need to hold her breath while the machine moves around her breast.
During a screening mammogram, there is usually just one technologist performing the test. For a diagnostic mammogram, however, a radiologist is often present so that he or she can review the images and decide if more pictures of specific areas of the breast are needed.
After a screening or diagnostic mammogram, a woman can resume her normal activities. The healthcare provider will call the patient within a few days to discuss the results of the mammogram and go over any next steps.
Patients diagnosed with breast cancer can find a team of experienced medical oncologists at Regional Cancer Care Associates. With more than twenty locations in New Jersey, Connecticut, Massachusetts, and the Washington, D.C., area, RCCA treats all cancer types, as well as benign and malignant blood disorders. The board-certified medical oncologists of RCCA use the latest advances in cancer care to create personalized plans for each patient. Treatment options include:
For more information about oncology care at RCCA or to request an appointment, contact us today.
For more information or to schedule an appointment,
call 844-346-7222. You can also schedule an appointment by calling the RCCA location nearest you.

“My uncle’s neighbor was diagnosed with the exact same cancer, I think, last year and his specialist has been wonderful. I’m going to get you

“What happens next?” “Where should I go for treatment?” They are questions physicians often hear after informing a patient that they have identified confirmed or
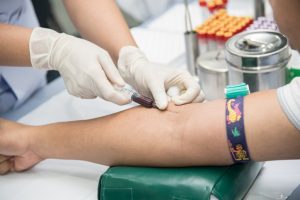
“You’re going to feel a little pinch.” Each year, tens of millions of Americans hear that phrase, or words to the same effect, just before

Regional Cancer Care Associates is one of fewer than 200 medical practices in the country selected to participate in the Oncology Care Model (OCM); a recent Medicare initiative aimed at improving care coordination and access to and quality of care for Medicare beneficiaries undergoing chemotherapy treatment.