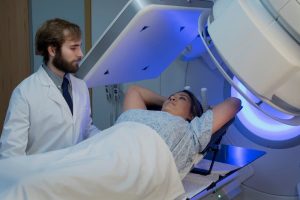
Radiation Therapy for Breast Cancer: How Does It Work?
Breast cancer is the second most common cancer affecting women in the United States, with only skin cancer occurring more often. Patients with breast cancer
HIPAA Alert: Potential Data Breach Learn More
Questions on Oncology, Hematology and/or Infusion Clinical Services due to COVID-19 Crisis – CALL 833-698-1623
Important Information for Our Patients Regarding the Coronavirus.
RCCA Providing Area Cancer Patients with Access to Care During Coronavirus Outbreak
RCCA Offering Patients Virtual Visits During Coronavirus Pandemic
The liver is a critical organ that performs many important functions, and discovering cancer in the liver can be overwhelming. Seeking treatment from experienced specialists like those at Regional Cancer Care Associates (RCCA) is crucial to obtaining the best possible outcome.
RCCA has a network of board-certified medical oncologists and hematologists with vast experience in caring for and treating patients with liver cancer. Because RCCA has more than 20 locations throughout New Jersey, Connecticut, Massachusetts, and the Washington, D.C., area, patients can access cutting-edge cancer care close to home.
The liver is the largest internal organ and is made up of various types of cells. Liver cancer occurs when these cells grow out of control. Different kinds of liver cells can turn into different types of tumors, both cancerous (malignant) and non-cancerous (benign). The treatment and prognosis will depend on the type of tumor.
The two main types of cancerous liver tumors are hepatocellular carcinoma (HCC) and cholangiocarcinoma.
HCC is the most common type of liver cancer in adults. It has different growth patterns, such as a singular tumor that grows larger and later spreads to other parts of the liver, or many smaller cancer nodules throughout the liver. A medical oncologist can classify the different subtypes of HCC, although typically the type will not affect the outlook or treatment plan.
The second most common type of liver cancer is called intrahepatic cholangiocarcinoma, or bile duct cancer. This type affects around 10 to 20 percent of patients with liver cancer, and it begins in the cells located in small bile ducts.
Several factors can increase a person’s risk of developing liver cancer. Many of these factors cause cirrhosis, a permanent scarring of the liver that is linked to an increased risk of cancer. These factors include:
Other risk factors are smoking cigarettes, using certain drugs (such as anabolic steroids), and having rare diseases like glycogen storage disease or Wilson’s disease. Losing weight, reducing alcohol consumption, and getting hepatitis vaccines and treatment can help reduce the chances of developing liver cancer.

Many types of cancer, including liver cancer, may not show initial signs and symptoms. As the cancer progresses, however, some symptoms may begin to appear, including:
People should keep in mind that many of these symptoms, particularly the early warning signs, may be due to other health issues. Speaking to a doctor is recommended if any of these symptoms persist or are severe.
With all cancer, early detection provides the best opportunity for effective treatment and good outcomes. However, because liver cancer may not cause symptoms at first, it can be challenging to diagnose the disease early. It may take a few doctor’s visits, tests, and scans to confirm the presence of cancer. Common diagnostic tests include:
Most people do not have to be screened for liver cancer. However, people with certain risk factors, such as a history of hepatitis B or C infections or liver cirrhosis, may receive recommendations from their providers for regular screening tests. An alpha-fetoprotein (AFP) tumor marker test may be recommended for patients with many or particularly worrisome risk factors. This test consists of having a blood draw and an ultrasound once or twice per year.
Once cancer has been diagnosis, determining its stage is imperative to determine the prognosis and appropriate course of treatment. Cancer staging is based on the location and extent of the cancer.
For hepatocellular carcinoma (HCC), medical oncologists often use the Barcelona Clinic Liver Cancer (BCLC) system to measure the size and spread of tumors. This system has five stages, from very early (0) to end-stage (D). The treatment plan developed will depend on the stage of the cancer.

The type and aggressiveness of cancer treatment will depend on the stage of the cancer as well as factors such as the patient’s overall health. Common treatments for liver cancer include:
Participating in clinical trials is also a possibility that can help treat liver cancer with innovative techniques. Regardless of the type or stage of cancer, the medical oncologists and hematologists at RCCA are with patients every step of their treatment journey.
Different cancer stages and types will have different prognoses – or outlooks – and additional factors such as the health, age, and gender of the patient can also affect the outlook. Generally, the earlier cancer is diagnosed, the better the prognosis because patients can start treatment right away to prevent the cancerous cells from spreading.
According to the American Cancer Society, the five-year relative survival rate for patients with liver cancer whose disease has not spread outside the liver is 36 percent. If the cancer has spread to other areas of the body, the percentage drops to 12 percent.
A liver cancer diagnosis can turn a person’s world upside down, but having a trusted team of medical oncologists working on your behalf can make the journey easier. At RCCA, oncologists and hematologists provide compassionate and comprehensive care for blood disorders and cancers like liver cancer. RCCA has more than 20 community-based locations across New Jersey, Connecticut, Massachusetts, and the Washington, D.C., area, so patients do not have to travel far from home for care. Contact RCCA today to schedule an appointment.
A liver cancer diagnosis is life-changing… for you and your loved ones. That makes it all the more vital that your care be advanced, your cancer care team be readily accessible, and your network of support be unfailing. At RCCA, these aspects of care, along with access to innovative clinical trials, are not “nice-to-haves” but rather “must-haves.” And they are the foundation of RCCA’s whole-person treatment philosophy.
For more information, or to schedule an appointment, call (844) 346-7222. You can also schedule an appointment by calling the RCCA location nearest you.

Breast cancer is the second most common cancer affecting women in the United States, with only skin cancer occurring more often. Patients with breast cancer

Colorectal cancer has been declining in the U.S. since the mid-1980s. However, incidents in adults younger than age 50 are rising. Though colorectal cancer is

New Jersey is home to some of the nation’s leading oncologists and hematologists, many of whom practice at Regional Cancer Care Associates (RCCA) treatment centers throughout the Garden State.
When standard cancer treatments aren’t providing the results you want, clinical trials may offer hope. Our physicians use clinical trials to study new treatments, helping transform cancer care for the better. You can enroll in a clinical trial to try groundbreaking treatment plans at zero cost to you.

Regional Cancer Care Associates is one of fewer than 200 medical practices in the country selected to participate in the Oncology Care Model (OCM); a recent Medicare initiative aimed at improving care coordination and access to and quality of care for Medicare beneficiaries undergoing chemotherapy treatment.